Filters
- BD Vacutainer (3)
- Chemistry test (1)
- Conventional Closure (1)
- Flow cytometry (1)
- Green Tubes (1)
- Hematology (1)
- Heparin Tubes (2)
- Plastic Tube (1)
- Sodium Heparin (9)
- Sodium Heparin Additive (2)
- Toxicology (2)
- Venous Blood Collection Tube (1)
- anticoagulant (3)
- Atrial fibrillation (1)
- blood clots (7)
- Blood clotting (1)
- blood thinner injection (1)
- Break up Blood Clots (11)
- cardiac surgery (2)
- Deep Vein Thrombosis (3)
- dialysis anticoagulant (1)
- doctor-only (17)
- Heparin 10000 unit (1)
- Heparin Sodium (13)
- Heparin-Induced Thrombocytopenia (1)
- hospital anticoagulant (1)
- intravenous Lines (1)
- IV heparin (1)
- Prevent Blood Clots (15)
- Prevention of clotting (1)
- pulmonary embolism (2)
- pulmonary embolism treatment (1)
- subcutaneous heparin (1)
- Surgical procedures (1)
- treatment of venous thrombosis (1)
- anticoagulant injection (1)
- blood clot prevention (1)
- Blood Thinner (6)
- DVT prevention (1)
- Heparin 5000 units (1)
- Heparin for IV (1)
- Heparin for IV catheter flushing (1)
- Heparin Injection (7)
- Hospital (1)
- Hypertension (5)
- Injectable heparin (1)
- PE prevention (1)
- Prevent Heart Attacks (5)
- Treat Hypertension (5)
- Venous thromboembolism (1)
- 71288-0404-05 (1)
- Heparin 40000 (1)
- Heparin Multiple Dose (1)
- Heparin IV Flush (4)
- Porcine (5)
- Prefilled Syringes (4)
- Arterial Blood Gases (1)
- Blood Sampling (1)
- Chemistry Panels (1)
- Electrolyte Testing (1)
- Plasma Determinations (1)
- 71288-0402-02 (1)
- Intravenous (1)
- Subcutaneous (1)
- Thin Blood (1)
- Blood Transfusions (4)
- Hemodialysis (4)
- Blood Clot Prevention (1)
- Blood Clot Treatment (1)
- DVT treatment (1)
- extracorporeal circulation (1)
- Hospital care (1)
Heparin Sodium Injections & Heparin IV Flush Solutions
Heparin sodium injection is a powerful anticoagulant (“blood thinner”) medication given by needle to prevent or treat blood clots. Heparin is a natural complex of sugar molecules (glycosaminoglycans) derived from animal sources (usually porcine intestine), standardized in units of activity. It cannot be taken by mouth (it would be broken down in the gut), so it is administered by injection – either intravenously (IV) or subcutaneously (under the skin). In clinical use, heparin injections rapidly reduce blood clotting ability to prevent new clots and keep existing clots from getting larger.
This injectable anticoagulant works immediately and is often used in hospitals or clinics for high-risk patients. For example, heparin injections are commonly given to bedridden or post-surgery patients to prevent deep vein thrombosis (DVT) and pulmonary embolism. Heparin is also used during certain medical procedures (like open-heart surgery, kidney dialysis, or blood transfusions) to stop the machine or process from causing clots. In short, heparin injections are life-saving treatments whenever rapidly thinning the blood is needed to prevent dangerous clots, but they require careful medical supervision because of bleeding risks.
Heparin sodium injection is an essential injectable anticoagulant used in many clinical situations to prevent or manage dangerous blood clots. Because it acts quickly and powerfully, it must be given carefully (by injection) and monitored closely. Always follow healthcare guidance when using heparin, and report any signs of bleeding or unusual symptoms immediately.
-
 Sale 30%
Original price $ 149.95Current price $ 104.50
Sale 30%
Original price $ 149.95Current price $ 104.50Sodium Heparin 10 mL Blood Collection Tubes, BD Vacutainer 16 mm x 100 mm, 100/box
BDNo reviewsSodium Heparin 10 mL blood collection tubes are used for collecting blood samples for tests that require plasma or whole blood. Sodium heparin acts...
View full details -
 Sale 27%
Original price $ 259.00Current price $ 189.00
Sale 27%
Original price $ 259.00Current price $ 189.00Heparin Sodium Injection 10,000 USP Multiple-Dose Glass Fliptop Vials 10 mL x 25/Pack (RX)
Pfizer Injectables2 reviewsTrusted Anticoagulant Solution for Deep Vein Thrombosis (DVT) Prophylaxis, Pulmonary Embolism Treatment, and Catheter Maintenance Experience premiu...
View full details🔒 Medical License Required -
 Sale 33%
Original price $ 87.95Current price $ 59.00
Sale 33%
Original price $ 87.95Current price $ 59.00Heparin Sodium Injection 5000 Units Per 1 mL Single Dose Vials 1 mL x 25/Pack (RX)
Meitheal PharmaceuticalsNo reviews#1 Hospital-Grade Anticoagulant for Blood Clot Prevention & Treatment Experience the gold standard in injectable anticoagulation with Heparin S...
View full details🔒 Medical License Required -
 Sale 39%
Original price $ 595.00Current price $ 365.00
Sale 39%
Original price $ 595.00Current price $ 365.00Heparin Sodium Injection 40000 Units Per 4 mL Multiple Dose Vials, 4 mL x 25/Pack (RX)
Meitheal PharmaceuticalsNo reviewsHeparin Sodium Injection is a medication used to prevent and treat blood clots in the veins, arteries, and lungs. It is also used to prevent blood ...
View full details🔒 Medical License Required -
 Sale 21%
Original price $ 99.95Current price $ 79.00
Sale 21%
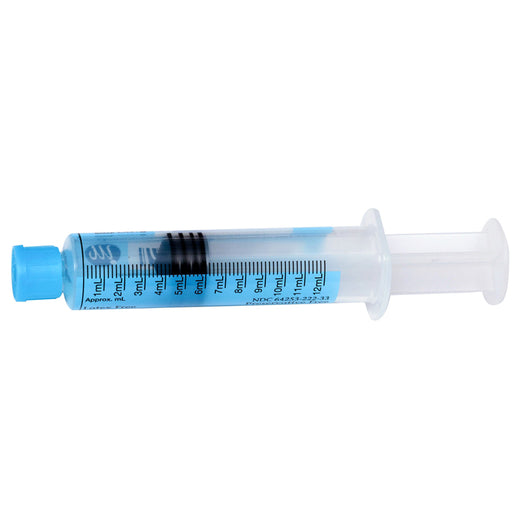
Original price $ 99.95Current price $ 79.00Heparin IV Flush Heparin Sodium, Porcine 10 U/mL Prefilled Flush Syringes 3 mL, 60/Box (Rx)
MedefilNo reviewsMedefil MIH-2233 Heparin IV Flush Heparin Sodium, Porcine Prefilled Flush Syringes 3 mL is sterile, single dose, disposable, plastic pre-filled sy...
View full details🔒 Medical License Required -
 Sale 31%
Original price $ 115.00Current price $ 79.00
Sale 31%
Original price $ 115.00Current price $ 79.00Sodium Heparin Blood Collection Tubes 6 mL BD Vacutainer, Green Cap, 13mm x 100mm, 100/box
BDNo reviewsSodium Heparin Blood Collection Tubes are used for collecting blood samples where plasma is required for testing. Sodium heparin acts as an anticoa...
View full details -
 Sale 27%
Original price $ 119.95Current price $ 87.00
Sale 27%
Original price $ 119.95Current price $ 87.00Heparin Sodium Injection USP 1000 Units Per 1 mL Single Dose Vials 1 mL x 25/Pack (RX)
Meitheal PharmaceuticalsNo reviewsHeparin Sodium Injection is a medication used to prevent and treat blood clots in the veins, arteries, and lungs. It is also used to prevent blood ...
View full details🔒 Medical License Required -
 Sale 16%
Original price $ 89.95Current price $ 75.95
Sale 16%
Original price $ 89.95Current price $ 75.95Heparin IV Flush Heparin Sodium, Porcine 100 U/mL Prefilled Flush Syringes 3 mL, 60/Box
MedefilNo reviewsMedefil MIH-3323 Heparin IV Flush Heparin Sodium, Porcine 100 U/mL Prefilled Flush Syringes 3 mL is sterile, single dose, disposable, plastic pre-...
View full details🔒 Medical License Required -
 Sale 29%
Original price $ 99.00Current price $ 69.95
Sale 29%
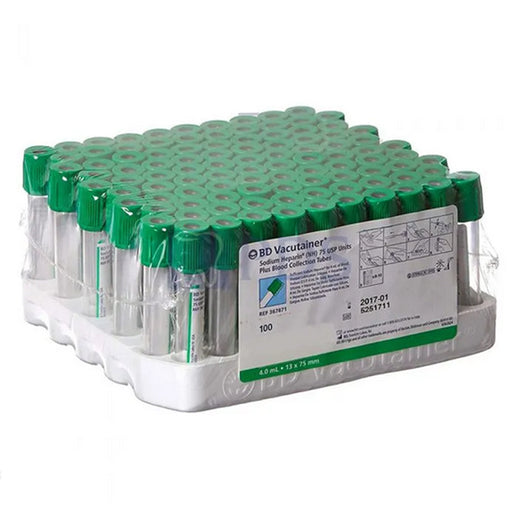
Original price $ 99.00Current price $ 69.95BD Vacutainer Sodium Heparin 4 mL Blood Collection Tubes 13mm x 75mm 100/Pack
BDNo reviewsBD 367871 Vacutainer® Plastic Heparin Tubes are used for plasma determinations in chemistry. The Tubes have a sodium heparin spray-coated at inne...
View full details -
 Sale 25%
Original price $ 79.95Current price $ 59.95
Sale 25%
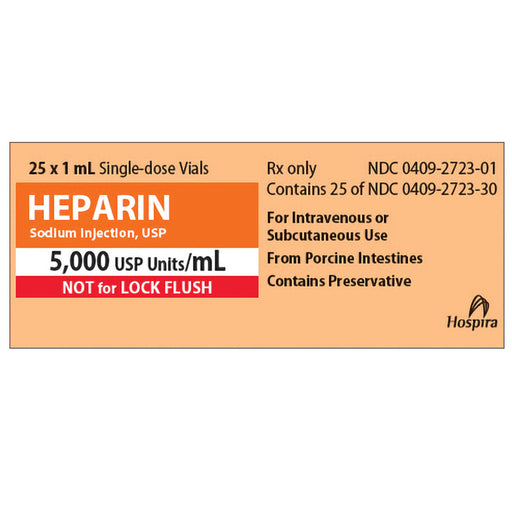
Original price $ 79.95Current price $ 59.95Heparin Sodium Injection 5000 Units Per 1 mL Single-Dose Vials 1 mL x 25/Pack (RX)
Pfizer InjectablesNo reviewsHeparin Sodium Injection 5000 Units Per 1 mL, Single-Dose Vials are a medication used to prevent and treat blood clots in the body. Each 1 mL vial ...
View full details🔒 Medical License Required -
 Sale 24%
Original price $ 229.95Current price $ 175.00
Sale 24%
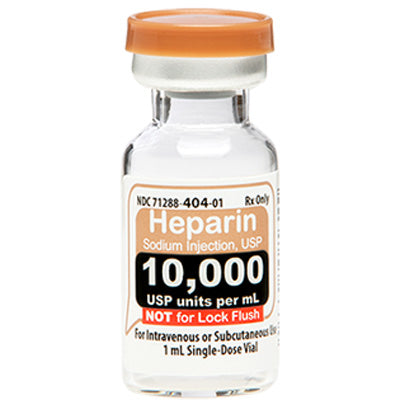
Original price $ 229.95Current price $ 175.00Heparin Sodium Injection USP 10000 Units Per 1 mL Single Dose Vials 1 mL x 25/Pack (RX)
Meitheal PharmaceuticalsNo reviewsHeparin Sodium Injection is a medication used to prevent and treat blood clots in the veins, arteries, and lungs. It is also used to prevent blood ...
View full details🔒 Medical License Required -
 Sale 23%
Original price $ 109.95Current price $ 84.95
Sale 23%
Original price $ 109.95Current price $ 84.95Heparin IV Flush Heparin Sodium, Porcine 100 U/mL Prefilled Flush Syringes 3 mL, 60/Box
MedefilNo reviewsMedefil MIH-3333 Heparin IV Flush Heparin Sodium, Porcine 100 U/mL Prefilled Flush Syringes 6 mL is sterile, single dose, disposable, plastic pre-...
View full details🔒 Medical License Required -
 Sale 22%
Original price $ 169.95Current price $ 132.00
Sale 22%
Original price $ 169.95Current price $ 132.00Heparin Sodium, Porcine 5000 Units Per mL Injection 1 mL Multiple-Dose Vials 25/Pack (RX)
McKesson Packaging ServicesNo reviewsNote; Not for Lock Flush. For intravenous or Subcutaneous use. Heparin Sodium, Porcine 5000 Units Per mL Injection 1 mL Multiple-Dose Vials is a me...
View full details🔒 Medical License Required -
 Sale 15%
Original price $ 539.95Current price $ 459.00
Sale 15%
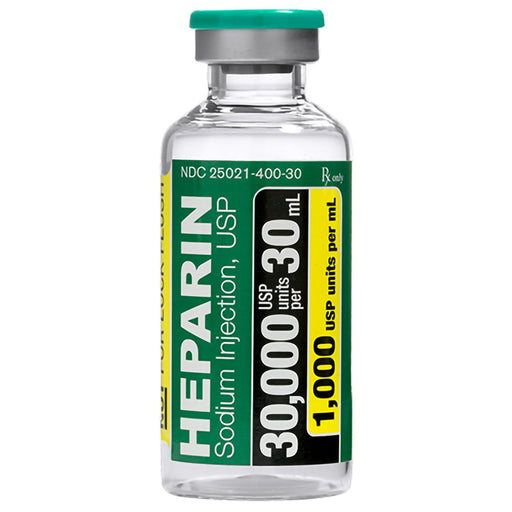
Original price $ 539.95Current price $ 459.00Heparin Sodium Porcine Injection 30000 Units Per 30 mL Multiple-Dose Vials 30 mL x 25/Pack by Sagent (RX)
Sagent PharmaceuticalsNo reviewsHeparin Sodium Porcine Injection is an injectable medication that contains the active ingredient heparin sodium, which is derived from pig intestin...
View full details🔒 Medical License Required -
 Sale 21%
Original price $ 999.95Current price $ 789.00
Sale 21%
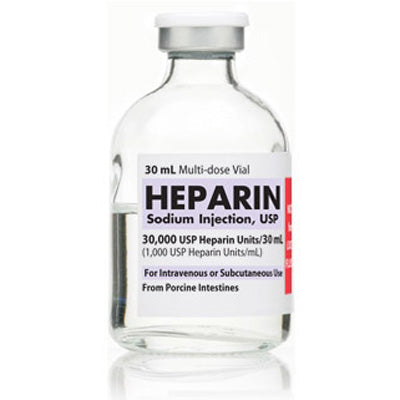
Original price $ 999.95Current price $ 789.00Heparin Sodium Injection 30000 Units Per 30 mL Multiple-Dose Vials 30 mL x 25/Pack (RX)
Pfizer InjectablesNo reviewsHeparin Sodium Injection is used to prevent and treat blood clots in the veins, arteries, and lungs. It is also used for certain procedures such as...
View full details🔒 Medical License Required -
 Sale 20%
Original price $ 105.95Current price $ 84.95
Sale 20%
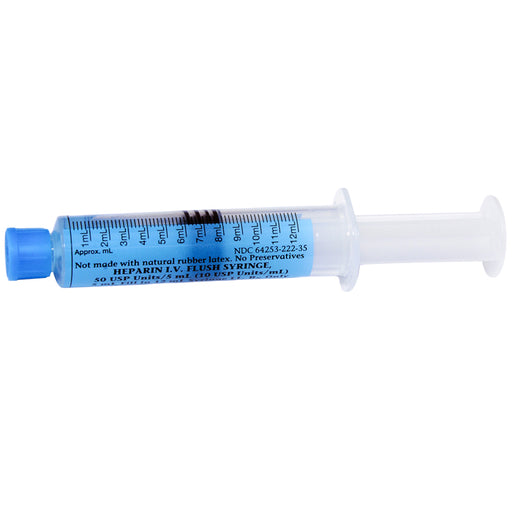
Original price $ 105.95Current price $ 84.95Heparin IV Flush Heparin Sodium, Porcine 10 U/mL Prefilled Flush Syringes 5 mL, 60/Box
MedefilNo reviewsMedefil MIH-2235 Heparin IV Flush Heparin Sodium, Porcine 10 U/mL Prefilled Flush Syringes 5 mL is sterile, single dose, disposable, plastic pre-f...
View full details🔒 Medical License Required -
 Sale 26%
Original price $ 189.95Current price $ 139.95
Sale 26%
Original price $ 189.95Current price $ 139.95Heparin Sodium Injection 10000 Units/mL Multiple-Dose Vials 10 mL25/Pack
Meitheal PharmaceuticalsNo reviewsHeparin Sodium Injection (10,000 units/mL) is a potent anticoagulant, often called a blood thinner, used for the prevention and treatment of blood ...
View full details🔒 Medical License Required -
 Sale 30%
Original price $ 135.00Current price $ 95.00
Sale 30%
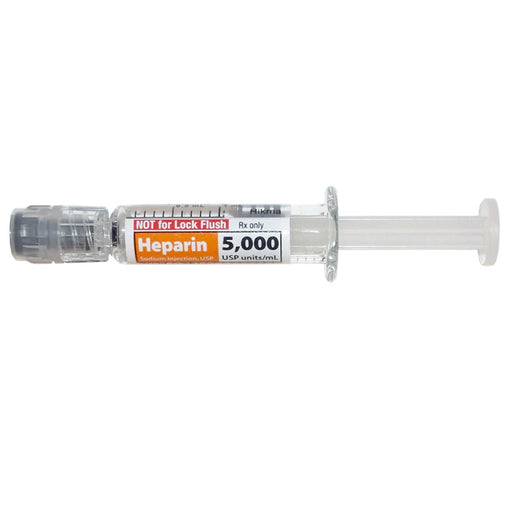
Original price $ 135.00Current price $ 95.00Heparin Sodium Injection Prefilled Syringes 5000 Units Per 1 mL x 25/Pack by Hikma (RX)
Hikma InjectablesNo reviewsHeparin Sodium Injection Prefilled Syringes 5000 Units Per 1 mL is a medication used to prevent and treat blood clots in the body. It contains the ...
View full details🔒 Medical License Required -
 Sale 14%
Original price $ 559.95Current price $ 479.00
Sale 14%
Original price $ 559.95Current price $ 479.00Heparin Sodium Injection USP 50000 Units Per 10 mL Multiple Dose Vials, 10 mL x 25/Pack (RX)
Meitheal PharmaceuticalsNo reviewsHeparin Sodium Injection is a medication used to prevent and treat blood clots in the veins, arteries, and lungs. It is also used to prevent blood ...
View full details🔒 Medical License Required -
 Sale 18%
Original price $ 145.95Current price $ 119.00
Sale 18%
Original price $ 145.95Current price $ 119.00Heparin Sodium Injection Prefilled Syringes 5000 Units Per 1 mL x 24/Pack by Meitheal (RX)
Meitheal PharmaceuticalNo reviewsHeparin Sodium Injection Prefilled Syringes 5000 Units Per 1 mL is a medication used to prevent and treat blood clots in the body. It contains the ...
View full details🔒 Medical License Required
People Also Searched For
Heparin sodium injection is a powerful anticoagulant (“blood thinner”) medication given by needle to prevent or treat blood clots. Heparin is a natural complex of sugar molecules (glycosaminoglycans) derived from animal sources (usually porcine intestine), standardized in units of activity. It cannot be taken by mouth (it would be broken down in the gut), so it is administered by injection – either intravenously (IV) or subcutaneously (under the skin). In clinical use, heparin injections rapidly reduce blood clotting ability to prevent new clots and keep existing clots from getting larger.
This injectable anticoagulant works immediately and is often used in hospitals or clinics for high-risk patients. For example, heparin injections are commonly given to bedridden or post-surgery patients to prevent deep vein thrombosis (DVT) and pulmonary embolism. Heparin is also used during certain medical procedures (like open-heart surgery, kidney dialysis, or blood transfusions) to stop the machine or process from causing clots. In short, heparin injections are life-saving treatments whenever rapidly thinning the blood is needed to prevent dangerous clots, but they require careful medical supervision because of bleeding risks.
Heparin sodium injection is an essential injectable anticoagulant used in many clinical situations to prevent or manage dangerous blood clots. Because it acts quickly and powerfully, it must be given carefully (by injection) and monitored closely. Always follow healthcare guidance when using heparin, and report any signs of bleeding or unusual symptoms immediately.
How Heparin Injections Work
Heparin enhances the body’s natural anticoagulant system. It binds to antithrombin III (AT III), a protein in the blood, and triggers a change that greatly increases AT III’s ability to inactivate clotting enzymes. In practice, this means heparin inhibits key factors in the clotting cascade – particularly Factor Xa and Factor IIa (thrombin). By blocking these enzymes, heparin prevents fibrin clots from forming and growing. (Importantly, heparin does not dissolve existing clots, it only prevents new clot formation or extension of current clots.
Because of this mechanism, heparin’s effect is immediate but short-lived. Clinicians often monitor blood clotting times (activated partial thromboplastin time, aPTT) to adjust dosing. High-dose heparin (e.g. via continuous IV drip) produces strong anticoagulation, while low-dose subcutaneous injections can provide mild anticoagulation for prophylaxis. Heparin’s activity is measured in units rather than milligrams; for example, many injectable vials come as 1 mL containing 10,000 units or more of heparin.
Indications – When Heparin Injections Are Used
Heparin sodium injections are indicated for a wide range of clot-related conditions. They include:
-
Preventing and treating venous clots such as deep vein thrombosis (DVT) and pulmonary embolism (PE). Patients at high risk of clots (e.g. after major abdominal or chest surgery, prolonged bed rest, or trauma) often receive heparin to prevent DVT/PE. Its use stops clots from forming in the legs or lungs.
-
Preventing clotting during surgeries and procedures. Heparin is used “bridge” during heart surgery or catheterization, or given during kidney dialysis and extracorporeal circulation to keep blood from clotting in the machine. For example, it is given routinely in cardiopulmonary bypass and angioplasty.
-
Cardiac conditions. In acute coronary syndromes (heart attack or unstable angina), heparin injection is used to reduce clot risk in the coronary arteries. It is also indicated in atrial fibrillation or flutter with embolization risk (to prevent stroke).
-
Disseminated intravascular coagulation (DIC). In some cases of severe systemic clotting (DIC), low-dose heparin can be used to interrupt the coagulation cascade.
-
Vascular procedures and devices. Heparin is used to prevent clotting in catheters, arterial lines, and blood transfusion equipment. (Note: flush solution for IV lines uses very dilute heparin, whereas therapeutic heparin injections are much higher strength.)
In practice, any situation where blood clots are likely – prophylactic or treatment – may call for heparin injection. (Key point: Heparin injection prevents clots but does not break down existing clots. For dissolving clots, other drugs (thrombolytics) are used instead.)
Administration and Dosing
Heparin sodium injections must be given by a healthcare professional (or by a trained patient, e.g. some pregnant women self-inject). It can be administered:
-
Intravenously (IV): A quick bolus (e.g. 5,000–10,000 units) can be given IV for immediate effect, often followed by a continuous IV infusion at a controlled rate (titrated to lab tests). This is the typical mode in intensive care or during procedures.
-
Subcutaneously (SC): For continued prophylaxis or longer-term treatment, heparin is often given by subcutaneous injection (usually in the abdominal fat). Typical regimens might involve two to three injections per day. For example, common dosing in adults is 8,000–15,000 units by deep subcutaneous injection every 8‒12 hours.
When giving subcutaneous heparin, the injection sites must be rotated to prevent hematomas and bruising. A different spot (usually on the abdomen) is used for each shot. It is injected deeply and slowly into fatty tissue; immediate massage is avoided to reduce local bleeding. Blood tests (aPTT) guide therapeutic dosing in high-dose therapy, since heparin levels can vary. (Low-dose prophylactic heparin may not always require monitoring in healthy patients.)
Heparin injection vials come in various strengths. A common concentration is 10,000 units/mL, but very concentrated vials (e.g. 50,000 units/10 mL) also exist. Important: These must not be confused with the much weaker heparin lock or flush solutions (10–100 units/mL) used to keep IV lines open – confusing them has been fatal.
Side Effects and Precautions
The biggest risk of heparin injection is bleeding. Since heparin prevents clotting, even minor injuries can lead to excessive bleeding. Hemorrhage is the chief complication: it can appear as easy bruising, bleeding gums, nosebleeds, or more serious internal bleeding (e.g. gastrointestinal or intracranial). Any sudden drop in blood pressure or unexplained weakness should prompt immediate evaluation (signs of bleeding). Patients on heparin must be monitored (bleeding, hemoglobin) and the dose adjusted carefully – even small dosing errors can cause over-anticoagulation.
Another serious side effect is Heparin-Induced Thrombocytopenia (HIT). In HIT, the immune system reacts to heparin-platelet complexes, dropping the platelet count and paradoxically increasing clot risk. This can occur 5–10 days after starting heparin. If HIT* is suspected (platelet count falls >50%, or thrombosis develops), heparin must be stopped immediately. A non-heparin anticoagulant (like argatroban or fondaparinux) is used instead. Patients with a history of HIT or heparin allergy should never receive heparin.
Injection site reactions are common but minor: pain, redness, warmth, itching or bruising where the needle was placed. These usually resolve on their own. Patients often notice some superficial bruising after subcutaneous shots. To minimize this, shallow (not intramuscular) injection is used.
Other adverse effects (usually with long-term high-dose use) include osteoporosis, alopecia (hair loss), and elevated liver enzymes. Rarely, skin necrosis or allergic reactions can occur. Because heparin can lower aldosterone, it may cause high potassium (hyperkalemia) – electrolytes may be monitored in prolonged therapy.
In practice, heparin therapy requires constant vigilance. Dose adjustments are made based on clotting tests (aPTT or anti-Xa levels) and patient response. Blood platelet counts are checked regularly (especially days 4–14) to catch HIT early. Before any invasive procedure or surgery, heparin is usually stopped or reversed with protamine sulfate (an antidote) to prevent uncontrollable bleeding.
Key Points
- Anticoagulant: Heparin sodium injection is a blood thinner used by injection to prevent and treat blood clots. It is a fast-acting shot or IV drip given in hospitals or by trained patients.
- Mechanism: It binds antithrombin III, blocking clotting factors IIa and Xa. It does not dissolve clots, only stops new clots/growth of existing ones.
- Route: Administered intravenously or subcutaneously – never by mouth. Subcutaneous injections (usually abdomen) must rotate sites. Dosing is weight-based and monitored by lab tests.
- Uses: Indicated for DVT/PE prevention and treatment, clot prevention after surgery, during heart attacks/unstable angina, in extracorporeal circuits (dialysis, bypass), atrial fibrillation with embolism risk, DIC, etc.
- Risks: Major risk is bleeding (any site, including brain or GI). Watch for unusual bruising or bleeding. A rare but dangerous complication is HIT (thrombocytopenia). Other side effects include injection-site pain/bruising and long-term effects like osteoporosis.
- Precautions: Use only under a doctor’s care. Notify providers of any bleeding or dental procedures. Heparin is not given to patients with active bleeding or certain conditions (e.g., severe hypertension) and requires lab monitoring.
How Heparin Injections Work
Heparin enhances the body’s natural anticoagulant system. It binds to antithrombin III (AT III), a protein in the blood, and triggers a change that greatly increases AT III’s ability to inactivate clotting enzymes. In practice, this means heparin inhibits key factors in the clotting cascade – particularly Factor Xa and Factor IIa (thrombin). By blocking these enzymes, heparin prevents fibrin clots from forming and growing. (Importantly, heparin does not dissolve existing clots, it only prevents new clot formation or extension of current clots.
Because of this mechanism, heparin’s effect is immediate but short-lived. Clinicians often monitor blood clotting times (activated partial thromboplastin time, aPTT) to adjust dosing. High-dose heparin (e.g. via continuous IV drip) produces strong anticoagulation, while low-dose subcutaneous injections can provide mild anticoagulation for prophylaxis. Heparin’s activity is measured in units rather than milligrams; for example, many injectable vials come as 1 mL containing 10,000 units or more of heparin.
Indications – When Heparin Injections Are Used
Heparin sodium injections are indicated for a wide range of clot-related conditions. They include:
-
Preventing and treating venous clots such as deep vein thrombosis (DVT) and pulmonary embolism (PE). Patients at high risk of clots (e.g. after major abdominal or chest surgery, prolonged bed rest, or trauma) often receive heparin to prevent DVT/PE. Its use stops clots from forming in the legs or lungs.
-
Preventing clotting during surgeries and procedures. Heparin is used “bridge” during heart surgery or catheterization, or given during kidney dialysis and extracorporeal circulation to keep blood from clotting in the machine. For example, it is given routinely in cardiopulmonary bypass and angioplasty.
-
Cardiac conditions. In acute coronary syndromes (heart attack or unstable angina), heparin injection is used to reduce clot risk in the coronary arteries. It is also indicated in atrial fibrillation or flutter with embolization risk (to prevent stroke).
-
Disseminated intravascular coagulation (DIC). In some cases of severe systemic clotting (DIC), low-dose heparin can be used to interrupt the coagulation cascade.
-
Vascular procedures and devices. Heparin is used to prevent clotting in catheters, arterial lines, and blood transfusion equipment. (Note: flush solution for IV lines uses very dilute heparin, whereas therapeutic heparin injections are much higher strength.)
In practice, any situation where blood clots are likely – prophylactic or treatment – may call for heparin injection. (Key point: Heparin injection prevents clots but does not break down existing clots. For dissolving clots, other drugs (thrombolytics) are used instead.)
Administration and Dosing
Heparin sodium injections must be given by a healthcare professional (or by a trained patient, e.g. some pregnant women self-inject). It can be administered:
-
Intravenously (IV): A quick bolus (e.g. 5,000–10,000 units) can be given IV for immediate effect, often followed by a continuous IV infusion at a controlled rate (titrated to lab tests). This is the typical mode in intensive care or during procedures.
-
Subcutaneously (SC): For continued prophylaxis or longer-term treatment, heparin is often given by subcutaneous injection (usually in the abdominal fat). Typical regimens might involve two to three injections per day. For example, common dosing in adults is 8,000–15,000 units by deep subcutaneous injection every 8‒12 hours.
When giving subcutaneous heparin, the injection sites must be rotated to prevent hematomas and bruising. A different spot (usually on the abdomen) is used for each shot. It is injected deeply and slowly into fatty tissue; immediate massage is avoided to reduce local bleeding. Blood tests (aPTT) guide therapeutic dosing in high-dose therapy, since heparin levels can vary. (Low-dose prophylactic heparin may not always require monitoring in healthy patients.)
Heparin injection vials come in various strengths. A common concentration is 10,000 units/mL, but very concentrated vials (e.g. 50,000 units/10 mL) also exist. Important: These must not be confused with the much weaker heparin lock or flush solutions (10–100 units/mL) used to keep IV lines open – confusing them has been fatal.
Side Effects and Precautions
The biggest risk of heparin injection is bleeding. Since heparin prevents clotting, even minor injuries can lead to excessive bleeding. Hemorrhage is the chief complication: it can appear as easy bruising, bleeding gums, nosebleeds, or more serious internal bleeding (e.g. gastrointestinal or intracranial). Any sudden drop in blood pressure or unexplained weakness should prompt immediate evaluation (signs of bleeding). Patients on heparin must be monitored (bleeding, hemoglobin) and the dose adjusted carefully – even small dosing errors can cause over-anticoagulation.
Another serious side effect is Heparin-Induced Thrombocytopenia (HIT). In HIT, the immune system reacts to heparin-platelet complexes, dropping the platelet count and paradoxically increasing clot risk. This can occur 5–10 days after starting heparin. If HIT* is suspected (platelet count falls >50%, or thrombosis develops), heparin must be stopped immediately. A non-heparin anticoagulant (like argatroban or fondaparinux) is used instead. Patients with a history of HIT or heparin allergy should never receive heparin.
Injection site reactions are common but minor: pain, redness, warmth, itching or bruising where the needle was placed. These usually resolve on their own. Patients often notice some superficial bruising after subcutaneous shots. To minimize this, shallow (not intramuscular) injection is used.
Other adverse effects (usually with long-term high-dose use) include osteoporosis, alopecia (hair loss), and elevated liver enzymes. Rarely, skin necrosis or allergic reactions can occur. Because heparin can lower aldosterone, it may cause high potassium (hyperkalemia) – electrolytes may be monitored in prolonged therapy.
In practice, heparin therapy requires constant vigilance. Dose adjustments are made based on clotting tests (aPTT or anti-Xa levels) and patient response. Blood platelet counts are checked regularly (especially days 4–14) to catch HIT early. Before any invasive procedure or surgery, heparin is usually stopped or reversed with protamine sulfate (an antidote) to prevent uncontrollable bleeding.
Key Points
- Anticoagulant: Heparin sodium injection is a blood thinner used by injection to prevent and treat blood clots. It is a fast-acting shot or IV drip given in hospitals or by trained patients.
- Mechanism: It binds antithrombin III, blocking clotting factors IIa and Xa. It does not dissolve clots, only stops new clots/growth of existing ones.
- Route: Administered intravenously or subcutaneously – never by mouth. Subcutaneous injections (usually abdomen) must rotate sites. Dosing is weight-based and monitored by lab tests.
- Uses: Indicated for DVT/PE prevention and treatment, clot prevention after surgery, during heart attacks/unstable angina, in extracorporeal circuits (dialysis, bypass), atrial fibrillation with embolism risk, DIC, etc.
- Risks: Major risk is bleeding (any site, including brain or GI). Watch for unusual bruising or bleeding. A rare but dangerous complication is HIT (thrombocytopenia). Other side effects include injection-site pain/bruising and long-term effects like osteoporosis.
- Precautions: Use only under a doctor’s care. Notify providers of any bleeding or dental procedures. Heparin is not given to patients with active bleeding or certain conditions (e.g., severe hypertension) and requires lab monitoring.




















